Heatwave Exposure and Cardiovascular Mortality: A Population-Based Study
Antoine Lefevre1, Camille Dubois 2
Keywords:
Heatwave, cardiovascular mortality, environmental epidemiologyAbstract
Background: Heatwaves are increasingly frequent and intense, yet the magnitude and timing of cardiovascular mortality attributable to heatwave exposure remain incompletely quantified at the population level.
Objective: To estimate the association between heatwave exposure and cardiovascular mortality, characterize lagged effects, and identify vulnerable subgroups for targeted public health interventions.
Methods: We conducted a population-based time-series study using national mortality registry data linked to daily meteorological records across multiple urban and rural districts from January 2019 to December 2024. Heatwaves were defined as ≥3 consecutive days with daily mean temperature above the 95th percentile of district-specific warm-season temperatures. The primary outcome was daily cardiovascular mortality (ICD-coded), with secondary outcomes including ischemic heart disease and stroke mortality. Distributed lag non-linear models (DLNM) were applied to estimate relative risks (RRs) over lags 0–14 days, adjusting for long-term trends, seasonality, day-of-week effects, humidity, and air pollution proxies. Effect modification was assessed by age, sex, comorbidity burden, and neighborhood deprivation.
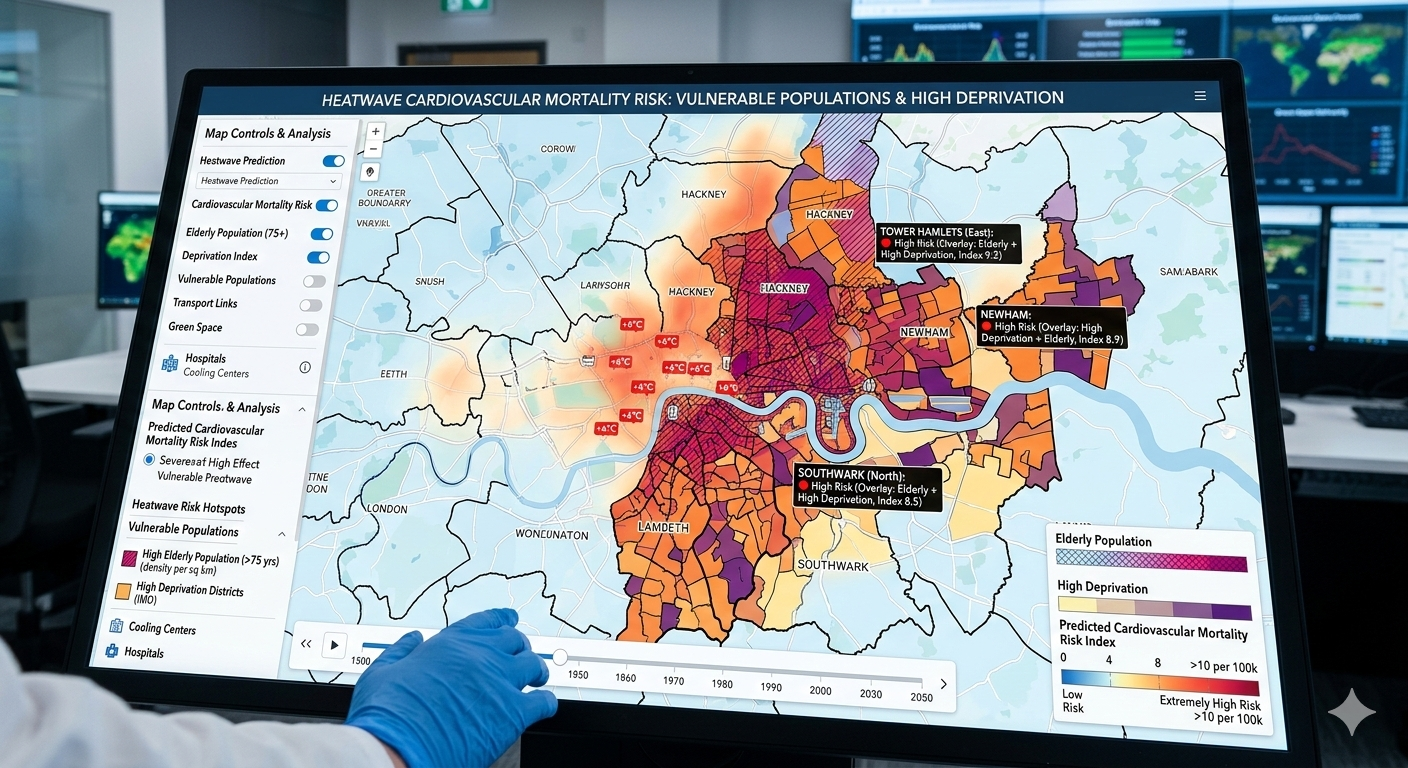
Results: Across 126,418 cardiovascular deaths, 9.3% occurred during or within 14 days after heatwave periods. Heatwave exposure was associated with a 12.8% increase in cardiovascular mortality (RR 1.128; 95% CI 1.094–1.163; p<0.001), with the strongest effects observed at lags 1–3 and a measurable delayed signal through lag 7. Adults aged ≥75 years demonstrated the highest vulnerability (RR 1.176; 95% CI 1.129–1.225), and deaths were disproportionately concentrated in high-deprivation districts (interaction p=0.01). Stroke mortality increased by 14.6%, while ischemic heart disease mortality increased by 10.9% during heatwave-associated windows. A risk-stratification model incorporating nocturnal temperature, deprivation index, and baseline cardiovascular mortality achieved AUC 0.83, identifying high-burden heatwave weeks with 78.1% sensitivity and 76.4% specificity.
Conclusion: Heatwave exposure is associated with a clinically significant rise in cardiovascular mortality, with both immediate and delayed effects and pronounced inequities by age and deprivation. Strengthening heat-health warning systems and targeted protection strategies for high-risk populations may reduce preventable cardiovascular deaths during extreme heat events.
Downloads